When I was new to interpreting, I would often find myself listening to the patient’s symptoms and making determinations (to myself, of course) as to what the diagnosis was.
Fever, pain with swallowing – strep throat!
Abdominal pain, worse after eating – gallstones!
Pain in feet, worse when walking barefoot – flat feet!
Not surprisingly, my diagnoses were frequently wrong, and so I came to realize that while I might know a lot of medical terms and concepts, I had no business trying to apply that knowledge beyond the accurate conversion of messages between languages.
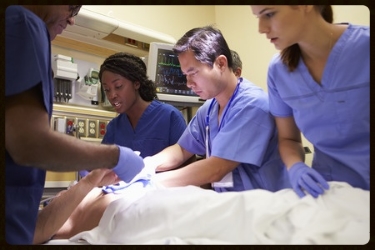
Any lingering delusions I had about my “medical abilities” dissipated one night at the Emergency Department. Long story short, the ED was arranging for the patient, a toddler, to be airlifted to a different hospital. In the meantime, the on-call pediatrician came to the ED for evaluation and consult. The pediatrician determined that the “abnormality” that alarmed the ED physician was not an abnormality after all. My lesson learned: I am infinitely less qualified to make a diagnosis (or treatment recommendation, or referral, or testing recommendation) than a credentialed ED physician. So, if an ED doc can get it wrong, I have no chance. And I need to remember that.
As interpreters, we learn a lot about biomedicine. It is a requirement expressed in the code of ethics because it supports our ability to interpret accurately and heightens our memory capacity. Still, I need to be careful to limit my application of medical knowledge to the communication of medical information and leave the diagnosing to the doctors. This boundary is also expressed in the interpreter’s ethics and for good reason.
So, hats off to the medical professionals and support staff who use their hard-earned skills and knowledge to the benefit of their patients and their patient’s families. As an interpreter, it’s a humble honor to use my skills so that they can use theirs.